Preimplantation genetic testing (PGT) is a cutting-edge procedure used to identify genetic abnormalities in embryos created with in vitro fertilization (IVF). The goal of PGT is to allow your physician to select embryos predicted to be free of a specific genetic condition or chromosome abnormalities for transfer. This test provides patients with an opportunity to reduce the chance for a genetic disease in their future children prior to pregnancy.
How it works
If you are interested in PGT, the first step is to notify your physician. Determining whether you should have PGT performed for your embryos is a complex decision so careful discussion with your physician is important. We also strongly recommend genetic counseling for all our patients who are considering PGT. Like all genetic tests, PGT has important benefits and limitations of which patients should be aware. The decision to have PGT needs to be made well in advance of your IVF cycle.
If PGT is part of your plan, you will need to undergo an IVF cycle to retrieve eggs and create embryos. The embryos are monitored in our laboratory until day 5 or 6 after fertilization when they are referred to as blastocysts. At that point, a small number of cells are removed from each embryo and shipped to an outside laboratory for PGT. The Fertility & Reproductive Center partners with several reference laboratories that perform PGT.
While PGT is being performed on the DNA from the cells that were removed, the embryos are cryopreserved (frozen) and stored in our laboratory. Once the PGT results are available, typically in 1-2 weeks after the biopsy, you will be notified of the results. If you have embryos that are appropriate for transfer, you will schedule a frozen embryo transfer with your physician.
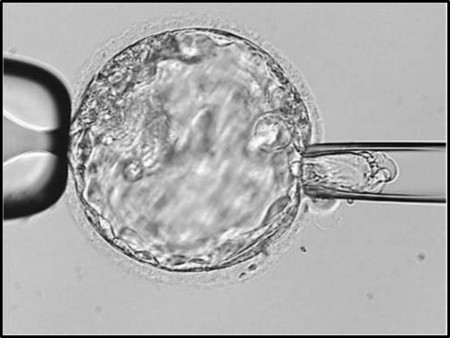
Testing to avoid inheritance of a single gene disorder (PGT-M)
Some patients seek IVF with PGT to reduce the chance of a specific genetic condition occurring in their children. This type of PGT is called preimplantation genetic testing for monogenic disorders (PGT-M). In some cases, the patient themselves may have a genetic condition such as neurofibromatosis type 1 or Marfan syndrome that could be passed on to their children. In other cases, both members of a couple may be carriers for a recessive genetic condition such as cystic fibrosis or sickle cell anemia, or the individual using their eggs may be a carrier for an X-linked condition such as Fragile X syndrome. HLA matching is also available for families with certain blood disorders who may wish for an embryo that could be an HLA match for a sibling or other family member.
Our physicians and genetic counselor work closely with such patients and an outside laboratory to design personalized testing for their embryos. The goal of PGT-M is to predict which embryos are free of the genetic condition for which they are at risk, allowing the physician to select those embryos for transfer. PGT-M can greatly reduce the risk of having an affected child prior to pregnancy.
Screening for chromosome abnormalities (PGT-A and PGT-SR)
PGT can also evaluate an embryo’s chromosomes, the structures in every cell that contain our genes. It is not uncommon for embryos have random chromosome abnormalities such as missing or extra chromosomes, also known as aneuploidy. Embryos with aneuploidy are more likely to result in a miscarriage or failed IVF cycle. Less commonly, aneuploidy may result in the birth of a child with a chromosome condition such as Down syndrome (trisomy 21).
In a typical IVF cycle, embryos are chosen for transfer based on their appearance under the microscope, which is referred to as their grade. The embryo’s appearance can give us some indication of its potential to result in a successful pregnancy, but it is not perfect. Preimplantation genetic testing for aneuploidy (PGT-A) provides additional information about the reproductive potential of the embryos and may help select the best embryo for transfer. PGT-A is most often considered for patient who have had recurrent pregnancy losses (miscarriages), multiple unexplained failed IVF cycles, a prior pregnancy or child with certain chromosome abnormalities, or based on the age of the individual providing their eggs. While PGT-A can be performed for any IVF cycle, there are both benefits and limitations that should be carefully discussed with your physician to determine if PGT-A is right for you.
One final type of PGT called PGT-SR is for structural rearrangements. This type of PGT is performed when a patient or their partner has a rearrangement of their own chromosomes such as a translocation or inversion. A person with a structural rearrangement of their own chromosomes is at increased risk to produce embryos with missing or extra pieces of chromosomes. Embryos with missing or extra pieces of chromosomes are more likely to result in a miscarriage or a child with serious health issues. PGT-SR can help to reduce those risks.
Questions?
If you would like additional information about PGT, you can find the answers to many frequently asked questions here.
If you have additional questions or feel PGT may be right for you, please contact us at 314.286.2497